Excellence in Helping Resolve Female Urological Issues
Our team of highly skilled urologists deliver expert care with compassion and sensitivity across the various urological symptoms that women experience. Urology for women covers a range of conditions and symptoms that can affect both men and women, but many of these are more prevalent in women. If you are experiencing uncomfortable or painful symptoms, we can help you get assistance to regain your urological health and wellbeing. Contact us today at 423-472-3201 for an appointment.
The Top 5 Gender-Specific Urinary Conditions in Women
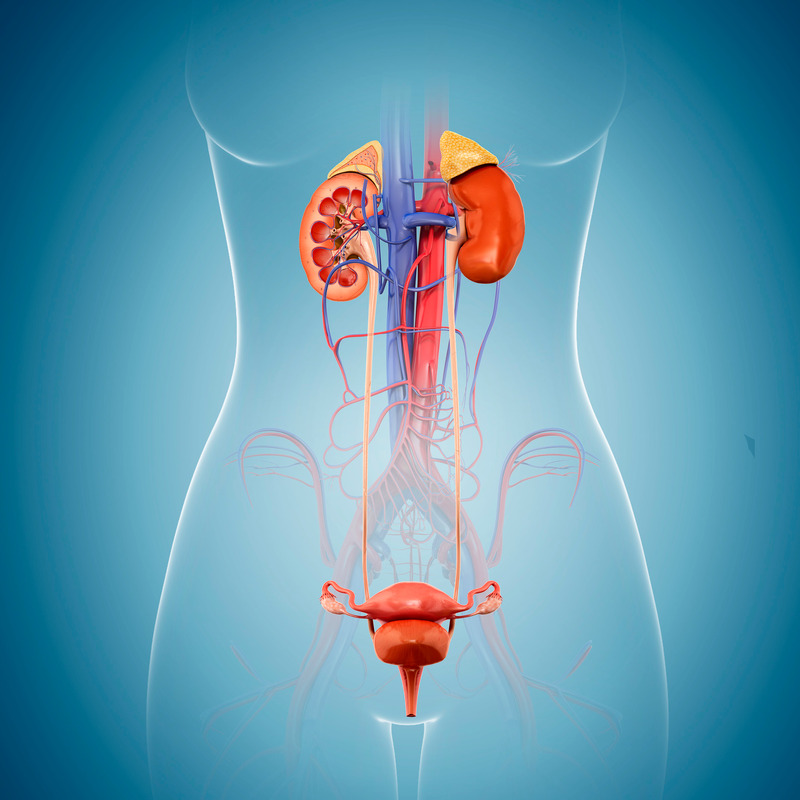
Female urology involves the treatment of many conditions that affect the urinary system. Some conditions occur more frequently in women than in men. Procedures for treating these conditions are the same as those in general urology. Some diseases occur in women only.
Conditions that occur in both sexes but are more common in women include:
We recommend a range of urology procedures to help women manage these conditions including:
The difference between women and men
A fundamental distinction between women and men is in their reproductive organs. In women, the reproductive system is separate from the urinary tract, so a gynecologist diagnoses and treats conditions that affect the reproductive organs. In men, the reproductive and urinary systems are more connected, so both are treated under the umbrella of urology.


The difference between female urology and gynecology
There are conditions affecting female reproductive health that have roots in an underlying urological condition and vice versa. One example is, interstitial cystitis, a urinary condition that can cause painful sexual intercourse. Alternatively, some urological problems are triggered by female reproductive processes, such as menopause which can lead to a urological disorder known as genitourinary syndrome of menopause.
Therefore it is important that an accurate diagnosis is made to allow urologists and gynecologists to effectively manage the condition appropriately and effectively in a collaborative manner.
Do You Have Questions? Speak To One Of Our Urology Experts!
Read more about gender specific urological conditions and procedures at:
Let's Discuss the Common Female Urology Conditions.
At Tennessee Valley Urology Center you can be confident in our quality of care.
Infections can affect any part of the urinary system, including kidneys, bladder ureters, and urethra. Urinary tract infections (UTIs) are more common in women because of the differences between female and male anatomy. In women, the urethra is shorter than in men, making it easier for the contaminating bacteria to get inside and cause infection. A chronic UTI is when the bacteria in the urinary system is difficult to treat, causing it to reoccur or to stay for longer than a few days.
A UTI usually starts in the bladder or urethra and then increases in severity until it causes pain in the pelvic region. Because the risk of infection increases with age, chronic UTIs are more common in older women. Multiple factors associated with ageing contribute to that risk.
Do you suffer chronic UTIs? It's a lot more than just recurring UTIs.
A bladder infection is a type of urinary tract infection (UTI). Some women are more vulnerable to contracting repeated UTIs, developing a condition known as chronic UTI. You may have chronic, or recurrent, bladder infections if you have two or more bladder infections in six months or three or
more infections in a year. There are several factors that can make women more likely to
have recurrent bladder infections. These factors include:
- Having kidney or bladder stones
- Bacteria get into the urethra (the passage that allows urine to exit the body) during sex
- Changing estrogen levels during menopause
- Problems with the urinary tract shape or function
- An inherited risk of developing bladder infections
Treatment is directed at the underlying cause, when possible. If you are experiencing UTIs often (more than 3 per year) you should see your healthcare provider. Your provider will want to do more test to find out the cause.

Female Specific Bladder Incontinence

Stress Incontinence
Stress incontinence is caused by a weakening of the pelvic floor muscles that help to hold the urine in the bladder. Any sudden pressure to the bladder, such as a sneeze or laugh, can then cause a leakage. Minimally invasive surgical correction of support can also correct stress incontinence.
The reason that stress incontinence is experienced more in women than in men is because of childbirth. Childbirth causes immense stress to muscles and nerves in the region between the legs, often bringing on stress incontinence. Fortunately, there are exercises called Kegel exercises that you can do to increase the strength of your pelvic floor region. Your urologist can tell you how to improve the results you see from these exercises so that you can enjoy a better outcome.
Overactive Bladder (OAB)
With an overactive bladder, the muscle that envelopes the bladder contracts involuntarily, which makes the pressure inside the bladder increase. If you have an overactive bladder, you may feel the urge to urinate frequently, but when you go to the toilet you will void small amounts. This is because the volume of the bladder has decreased.
An overactive bladder is not painful but can alter your lifestyle. The frequent trips to the toilet during the night or the interruptions to your daily schedule can quickly become a nuisance. Fortunately, urologists can recommend several treatments that will help normalize frequency, urgency, and night time trips to void.
Pelvic Organ Prolapse
Pelvic organ prolapse can be a distressing condition as it occurs when the muscles and tissues in the pelvic cavity become too weak to support the pelvic organs (bladder, uterus or colon). This causes the organs to drop, putting pressure on the vagina and causing those organs to prolapse or even protrude.This condition is not dangerous, but it can be painful and reduce your quality of life. Occasionally medical treatment is necessary to correct it, but the symptoms can often be improved with pelvic floor exercises (Kegel exercises) or other treatments that your urologist will explain to you.
Some women may be reluctant to discuss their symptoms of pelvic organ prolapse; however, this type of condition is very treatable. Sometimes, women may suffer both pelvic organ prolapse with urinary incontinence, so it is important you speak with your urology specialist to get the help you need.
Interstitial Cystitis (IC) ~ Painful Bladder Syndrome
Interstitial cystitis (IC) involves chronic recurrent pain or pressure in the bladder or pelvic area. It’s also known as painful bladder syndrome and bladder pain syndrome. If you have IC, you will notice that you get temporary relief from the pain after going to the toilet to urinate. You may also notice that the intensity of pain fluctuates from weeks to months. These symptom fluctuations may be caused by lifestyle or dietary changes.

Is Interstitial Cystitis an Infection?
IC is not an infection, and so can’t be treated with antibiotics. That’s why it’s important to see your urologist to learn about all the available options to reduce pain and increase quality of life with this condition.
How is IC Diagnosed?
Interstitial cystitis is tricky to diagnose, so your urologist may conduct a variety of tests to rule out infection or other conditions.

Treatment Options for IC
Once IC is established, your doctor will decide the best treatment based on your symptoms and other health issues, such as:
- Lifestyle changes, diet and exercise
- Oral medication
- Physical therapy
- Bladder training
- Nerve stimulation
Female Urology Procedures
There are several urological procedures that can be specific to the female anatomy or are more common in women rather than men. For more information on procedures for both men and women see our General Urology procedures.

Pelvic Floor Rehabilitiation
Pelvic floor rehabilitation can help women with urinary incontinence, giving them the skills they need to take back control of their bladder. Kegel exercises (invented by Dr. Arnold H. Kegel in the 1940s) can be done to help in strengthening the pelvic floor muscles. Kegels can be done by contracting (squeezing) and relaxing the pelvic floor muscles several times a day.
The pelvic floor is a group of muscles that support the reproductive and urinary tract system. When the muscles are not performing like they should, this can cause issues such as pain and symptoms that could affect your daily life.
To ensure you are performing the exercises correctly, your provider may refer you to pelvic floor therapy. Physical therapy can help in easing pain and symptoms. Ask your healthcare provider about pelvic floor rehabilitation for more information.
Bladder Sling or "Sling Surgery"
The most common procedure for SUI is the “sling surgery.” This minimally invasive procedure is estimated to only take 20-30 minutes. A small incision will be made in the vaginal area. Next, the synthetic mesh implant is placed to create a “sling” of support under the urethra. After the position is correct, your physician will close and bandage the small incision in the groin area (if applicable for your sling type) and the top of the vaginal canal.
Mid-urethral slings have been studied since the mid-1990’s and have shown to have a high success rate of 80-95%. Most women will see improvement immediately after the procedure. Talk to your physician about what you should expect.
The Bladder Sling is a type of ‘hammock’ surgically placed into your pelvic area to help with urinary incontinence. It loops under the neck of the bladder to create a light pressure, increase the force of your pelvic floor muscles and maximize your chances of keeping the urine in the bladder until you get to the toilet.

Got Questions? Want to Speak to one of our Urology Experts?
We Offer Women Sensitive and Compassionate Care for their Urology Symptoms
Our highly skilled, board-certified Urology specialists are the leading urology doctors across the Tennessee Valley. Call Tennessee Valley Urology Center today to book your appointment and visit us at our Cleveland or Athens offices. You can be confident in a urological consult with one of our providers to discuss your unique symptoms and treatment plan
Helping Patients In and Around Cleveland TN
- Benton
- Hopewell
- McDonald
- Ocoee
- Ooltewah
- Reliance
- Snow Hill
- South Cleveland
- Wildwood Lake
Supporting Patients In and Around Athens TN
- Decatur
- Etowah
- Madisonville
- Niota
- Riceville
- Sweetwater
- Williamsburg
Treating Patients In and Around Copper Basin & GA, NC Border Towns
- Ducktown
- Harbuck
- Wildwater
- Blue Ridge
- Mccaysville
- Murphy

